
Hira Health: Guiding Cancer Care
Conceptualized a wearable companion to help patients navigate cancer care at UPMC Magee-Womens Hospital.
Our Challenge
Gynecologic oncology care is clinically excellent, but it can still feel confusing, isolating, and overwhelming.
We partnered with UPMC Magee-Womens Hospital on a 15-week project exploring care coordination in gynecologic oncology across appointments, handoffs, and everything in between.
Through appointment shadowing, provider observation, and co-design with patients, caregivers, and clinicians, I mapped where support breaks down and what more navigable care could look like.
After hearing so many women describe spending their lives caring for others, it was clear that care should not be asking them to stay strong in silence. It should be giving them space to speak about what is real.
The Patient Journey
Observing appointments firsthand showed us exactly where support breaks down and anxiety builds.
To find where support could have the greatest impact, we shadowed appointments, observed provider charting, and sat in waiting rooms at UPMC. What emerged was a critical inflection point: the appointment itself.
This is where knowledge transfers, treatment paths shift, and understanding can change in minutes. Patients walk in with questions they've rehearsed for days. They walk out struggling to recall the answers.
Pre Appt.
The Waiting Room
Anxiety builds before the visit
Remember questions and symptoms
A place to prepare without pressure
During Appt.
Inside the Exam Room
Information moves too fast
Ask the right questions in the moment
Capture what matters quietly
Post Appt.
Leaving the Visit
Details blur after the visit
Make sense of next steps and updates
Clear talking points to revisit
Framing the Opportunity
How might we help patients capture, organize, and revisit what matters before, during, and after appointments?
The problem wasn't a lack of care, it was a lack of continuity. Patients needed a way to hold onto fleeting moments and carry them into the next conversation.
Explored Directions
We mapped out possible directions, weighing tradeoffs across patient effort and contextual fit.
We ran several activities that helped us find trends in our research and pinpoint a solution where we could help patients capture, organize, and revisit what matters.
After brainstorming themes, we organized a rough mind map to see the potential of different ideas and discussed the pros and cons of each direction based on our findings.
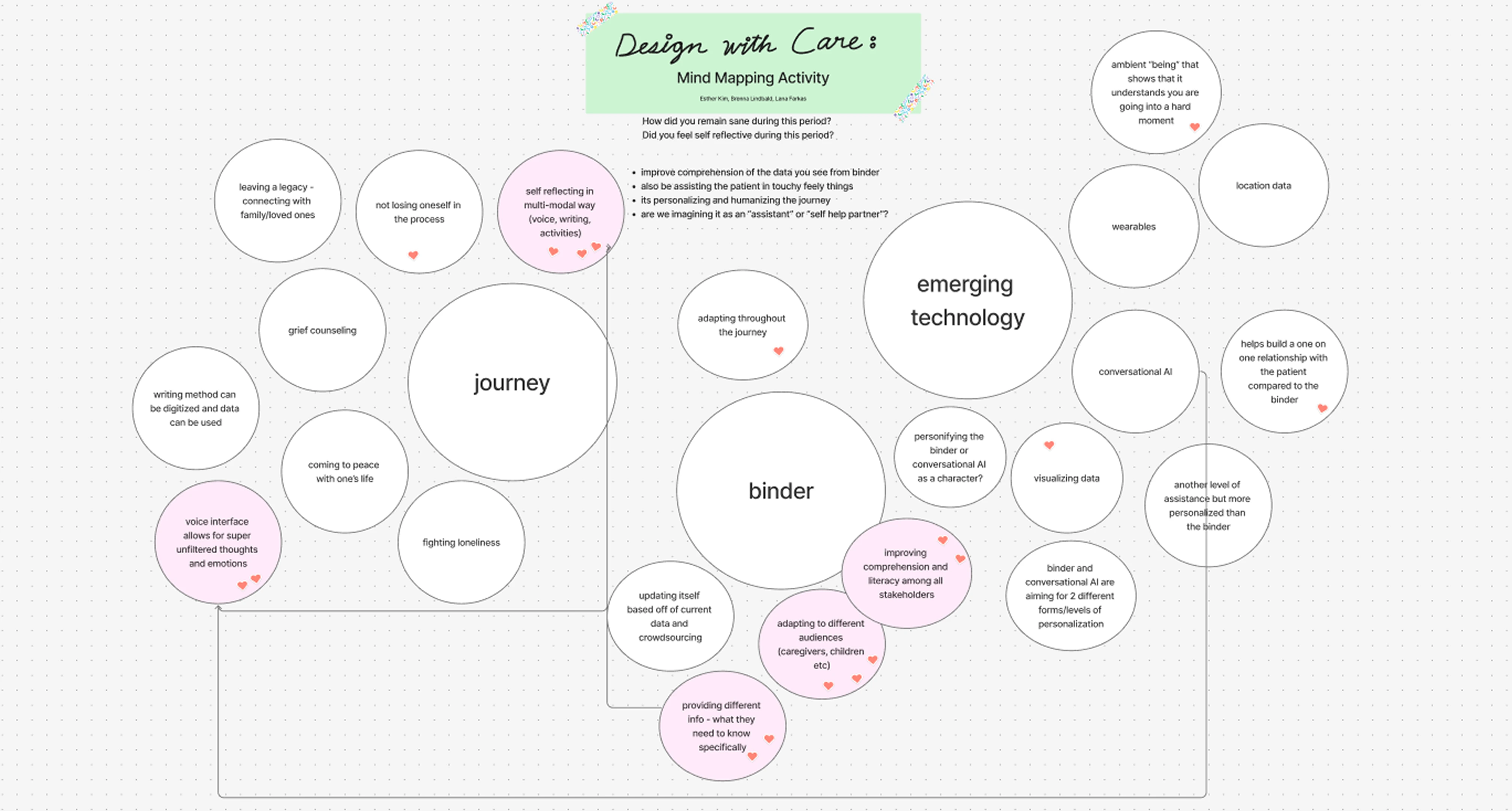
Finding clarity through a brain dump!
Where We Landed
A listening-first wearable that helps patients capture what matters without adding friction.
We explored different ways to embed support into cancer care, and ultimately landed on an ambient listening wearable as lightweight capture that adds richer context patients can use in the moment and revisit later.
Why a Wearable?

Biometrics, time, and location add signal to symptoms and patterns across appointments.
Why Voice?

Speaking preserves emotion and nuance that gets lost in typed notes when energy is limited.
Why Recording?

Creates a reviewable history for talking points and next steps without relying on memory.
Testing Our Concept
We brought our early concept back to UPMC to pressure-test it with patients, caregivers, and providers.
With an ambient listening tool as our starting direction, we facilitated a co-design workshop with patients, caregivers, and healthcare providers. We wanted to understand what support should sound like, feel like, and do across the appointment journey.

Experience Mapping
Participants mapped how they felt across appointments and what they wished they could hear in those moments.

Desired Support Systems
Using cutout templates, participants designed their ideal "virtual caregiver" with qualities they’d want during treatment.
What We Heard
Everyone wanted something different, but one theme kept surfacing. Patients just wanted to be heard.
We heard a wide range of needs, but the strongest signal was simpler than we expected. Patients didn’t need another voice telling them what to do. They needed to feel heard, understood, and in control of their own experience.
This realization pushed us to rethink our approach. The answer wasn’t a smarter system. It was a simpler one.
Product Pivot
We shifted from a tool that responds to one that reflects what patients already know.
Our original concept responded with suggestions based on what it heard. But patients didn’t want more advice. They wanted their own thoughts captured and surfaced when it mattered.
So we pivoted. Hira still prompts, but through questions, not assumptions. It invites reflection rather than prescribing action, and the meaning stays yours to define.
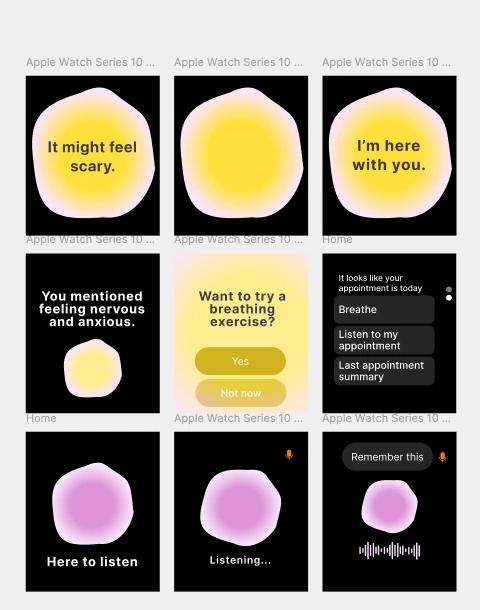

Final Solution
Meet Hira, A WatchOS tool designed to help patients feel heard, stay grounded, and leave appointments with clarity.
1. Say it out loud to capture a moment
Record a quick thought or symptom without interrupting what you're doing.
2. Surface prompts, reminders, and recent logs
Swipe through widgets that keep priorities visible: what's next, what's new, what repeats.
3. Review your patterns to prep for what's next
Turn voice logs into themes you can revisit before appointments and significant decisions.
Live Context
Hira uses context signals to nudge at the right moments with gentle reminders, check-ins, and prep.
Mobile Companion
Hira's mobile view brings everything together, including appointments, health signals, and long-term trends.
1. Sync appointments and health data
Sync appointments from the hospital portal and biometrics from Apple Health for richer context.
2. Track patterns across days and weeks
Visualize symptom trends and recurring themes pulled from voice-logged notes.
External Review
A live demo and Q&A helped us validate what resonated and what needed tighter framing.
In our end of year review, we shared the concept and safety boundaries with invited health professionals, and used their feedback to clarify Hira as a recall-and-follow-through tool.
"I can see this being huge, especially for patients who don't have anyone to go with them to appointments."
"This is exactly what patient care needs right now. Plus it's helpful for doctors too. Please keep on building."
Perceived Impact
Tools like Hira matter because support systems aren't always there when they should be.
When support systems fall short, small moments can carry a lot of weight. Throughout our research, we heard about patients managing treatment alone and caregivers doing everything they can.
Hira can't replace human connection, but it can hold space when no one else is around.
We can't solve systemic inequities with a product, but we can build something that meets people where they are and gives them one less thing to carry alone.
What I Learned
The hard conversations were the ones that mattered most, and they shaped everything we built.
Designing for cancer care meant sitting with discomfort and asking questions that didn't have easy answers. Those conversations were heavy, but they were also the reason we arrived at something real.
Sometimes the answer to a complex problem is a simple solution that adapts. Not every moment needs a response. Some just need to be held, and I’ll carry that lesson forward as I keep designing with more intention.
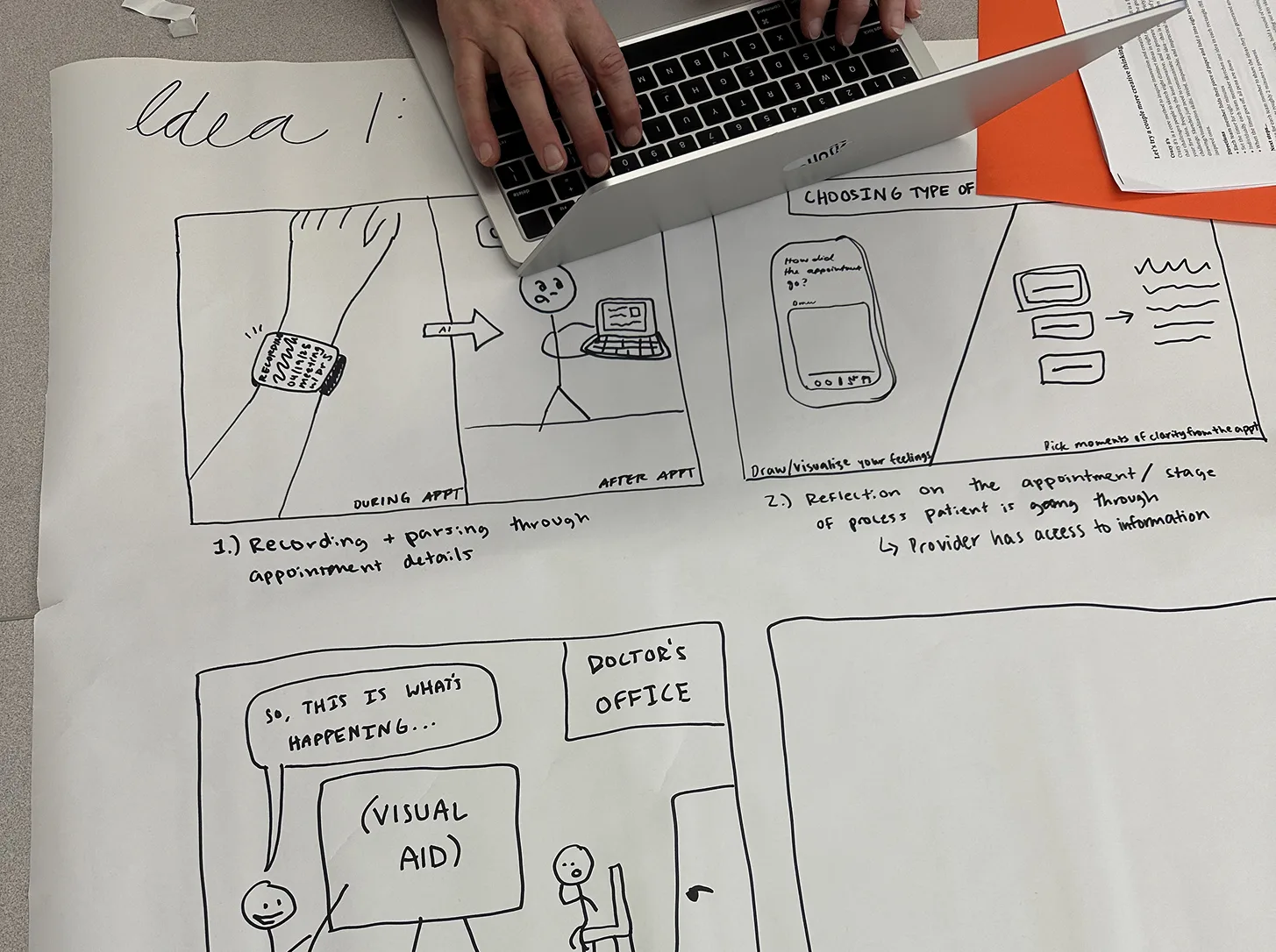
Storyboarding our way through the hard parts...

Designing with care, and a lot of critique!








